Blood- restricting bands, smart inhalers, teletherapy are some of the groundbreaking technologies that will change the medical world forever.
Healthcare is something that is constantly changing. New technologies and capabilities enhance abilities for doctors and researches. New treatments become available, which greatly benefit the medical industry.
These are some of the things which we can expect in 2024.

Smart inhalers
Inhaled corticosteroids and bronchodilators are one of the most important treatments for asthma.
The first one helps control inflammation while the second provides instant relief when symptoms start.
They are efficient when used correctly, but up to 94 percent of people don’t use them correctly.
“Standard of care works for approximately 90 percent of all patients when taken correctly and as prescribed,” Tonya A. Winders, president and chief executive officer of the Allergy & Asthma Network, told Healthline.
“On the other hand, studies show that about 50 percent of patients with asthma is not well controlled, which leads us to believe more can be done to increase adherence.”
This is where blue-tooth enabled smart inhalers to come in.
These devices help detect inhaler use, remind patients that they need to use their medication, encourage proper use of the device, and help the patient’s general use of the inhaler by collecting data from the device
Every time the inhaler is used, it records the date, time, place, and if the dose was properly taken.
“This will provide valuable insight to determine how adherent patients are to their controller medications, as well as help us understand the patterns of when a patient experiences a flare,” Winders said.
These devices which clip to the existing inhalers and send data to a smartphone app are available right now.
A clinical trial for Propeller’s add-on smart inhaler device showed that participants used less reliever medication, had more reliever-free days, and improved overall asthma control over the course of one year.
The first fully integrated smart inhalers will be available by the middle of the year, according to Winders

Blood flow restriction training
One of the biggest fitness innovations for 2018 promises big muscle growth results while using as little as 10 to 20 percent of the weight you’d typically use.
How might you ask?
By restricting your blood flow.
Blood flow restriction (BFR) training uses specialized blood pressure cuffs or bands to prevent the flow of oxygen-deprived blood out of your limbs.
When your blood pressure reaches optimal levels, you perform traditional muscle-building maneuvers, but you use smaller weights.
A study in the Journal of Applied Physiology found that this kind of training increases muscle tone while using loads lighter than 20 percent of your one-rep max.
Research shows that by restricting the blood flow, you reduce the oxygen your muscles can access during the exercise.
Your muscles go into metabolic stress without the oxygen.
You don’t need heavy weights to shock your muscles into growth while they’re in the low-oxygen phase.
Dr. William P. Kelley, DPT, ATC, CSCS, with USA Sports Therapy, advises that you consult someone trained to properly perform BFR, before going to the gym with a band or a strap.
“You should absolutely only do BFR training with someone who is a certified BFR clinician,” said Kelley for Healthline.
What could happen you try BFR by yourself?
Kelley said it’ can cause nerve or vascular damage if done incorrectly or without proper training and supervision and with subpar equipment,”

Teletherapy
Smartphone apps and chatbots are causing quite a stir in the therapy field, but it’s another technology that might bring human-to-human interaction back with mental health treatments.
Dr. Ken Duckworth, medical director for the National Alliance on Mental Illness, said that “Teletherapy, or delivering sessions by a video-enabled interface, is probably the most important tech development for mental health,”
He also told Healthline that as society becomes more educated about the role of mental healthcare in overall care, the demand will be greater on therapists and psychiatrists.
The reality is, the number of these providers isn’t growing to meet the demand of patients.
One of this platforms is yourdoctors.online.
The benefits of this web-based experience are that no one has to travel, and you can have a session whenever you want, and wherever you are.
“The core problem with mental health is that the demand exceeds the supply. So, the question is, how does the technology work to deliver people those same services?” said Duckworth.
Teletherapy is almost the same as a traditional therapy in every way.
You still sit face-to-face with a practitioner, and you talk or chat with him/her.
In this case, instead of a chair or a couch, you use professional service.
“The no-show rates are lower. You might be able to have people on the East Coast seeing people on the West Coast at different times of the day,” Duckworth said. “You’re providing the same service, in a more efficient way.”
The uptake for teletherapy is slow right now, but many believe that it will quickly speed up as people become more familiar with the benefits.
“I think this is a cultural evolution and I think it’s going to take some time,” he said.
Precision meds for cancer treatment
More than 1.6 million people will be diagnosed with cancer in 2018.
Those people have the tools to find cancer which are better than ever.
One of those tools is precision medicine, according to Dr. Otis Brawley, MACP, chief medical director and scientific officer of the American Cancer Society.
Precision medicine allows doctors to select medicines based on individual cancer’s genetic makeup.
In plain English, doctors won’t just treat lung cancer. They will be able to treat the type of lung cancer you have, down to the specific abnormal genes and proteins.
“Instead of a particular organ system cancer, we’ll be looking at cancer and then what is the molecular thing that we can exploit in that cancer,” said Brawley.
Precision medicine is not the cure, however. Scientists and doctors like Brawley see great hope that one day, they will be able to tailor treatments to each cancer’s genetic traits and changes.
The hope is that precision medicines will become better and doctors will use them where they are able to.
“If we can get better at utilizing these precision medicines, we’ll actually be able to cure some solid metastatic tumors,” Brawley said.
Brawley also told Healthline, “Over the years, we’ve gained a greater understanding of what’s going on inside a cell as it becomes cancerous and once it is cancerous. Inside the cell, there are certain molecular mechanisms, certain genetic mutations, that make it vulnerable for treatment.”
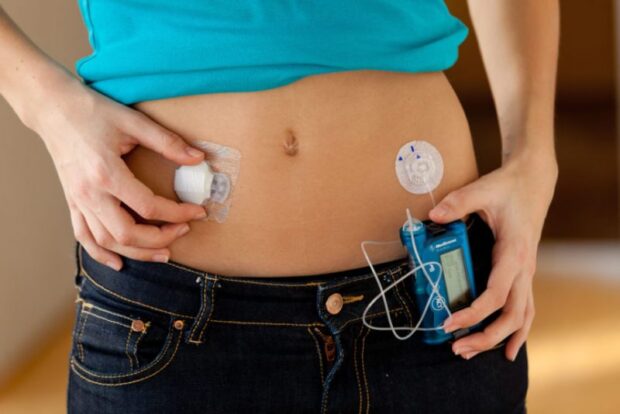
Artificial Pancreas
Every year, medical technology companies are working to make diabetes more hands-off, end the dreaded cycle of checking and monitoring, and streamline the glucose-delivery process.
They are getting closer with artificial pancreases, or better known as automated insulin delivery systems.
These systems, worn like traditional insulin pumps, are designed to make the blood-sugar management automated by monitoring glucose levels continuously and providing insulin that can stabilize blood sugar levels.
This is all managed by an algorithm that connects your insulin pump and the artificial pancreas to a smartphone.
“It can detect what your glucose level is, and it has an insulin delivery device that can deliver subcutaneous insulin instantly,” Dr. Robert Courgi, an endocrinologist and hospitalist with Northwell Health in New York, told Healthline. He also added, “That smart technology can change and vary as needed, instead of giving you that one fixed-dose constantly.”
The U.S. Food and Drug Administration (FDA) approved the first “closed-loop” system of this kind in 2016.
While it has been available for more than a year, newer versions are anticipated in the upcoming months and years.
T Dr. Mark D. DeBoer, associate professor of pediatrics in the pediatric endocrinology division at the University of Virginia, said that these new versions would hopefully deliver greater ease of use and satisfaction.
“What most children and adolescents are seeking in an artificial pancreas system is one that overall decreases the work that they put into their diabetes. The ideal system for patients with diabetes is to ‘set and forget,’ and we are not there yet,” DeBoer also told Healthline.
“Patients still need to be aware of what their blood sugars are and what the system is doing, but we are hoping that more work and research in the field will keep moving toward wider use.”
This kind of medical marvel took decades because of the complexity, according to Dr. Gerald Bernstein, an endocrinologist and coordinator of the Friedman Diabetes Institute at Lenox Hill Hospital in New York City.
He said that even though we have advanced, we have a long way to go before we can replicate human pancreases.
“We got to the moon and have rocket ships that can go back and forth, all before we were able to create anything close to an artificial pancreas because of the complexity”, Bernstein told Healthline. “Now we have to see if the algorithm will hold up over time.”
 Comeau Computing Tech Magazine 2024
Comeau Computing Tech Magazine 2024